Our programs and priorities
We’re focused on addressing South Eastern NSW's health challenges and emerging areas of critical importance. We offer a range of programs, services and information for the health priorities and needs of the region.
Tools and resources for general practice
We provide support to general practices across the region to improve quality of care and to access the latest technology, resources and education.
-

Accreditation
Find out moreWe are dedicated to supporting general practices across our region to achieve and maintain accreditation status.
-

Cancer screening
Find out moreWe work with general practices to improve screening participation rates and reduce the risk of cancers.
-

Data quality
Find out moreWe work with general practices to improve the overall effectiveness of routine primary care consultations.
-
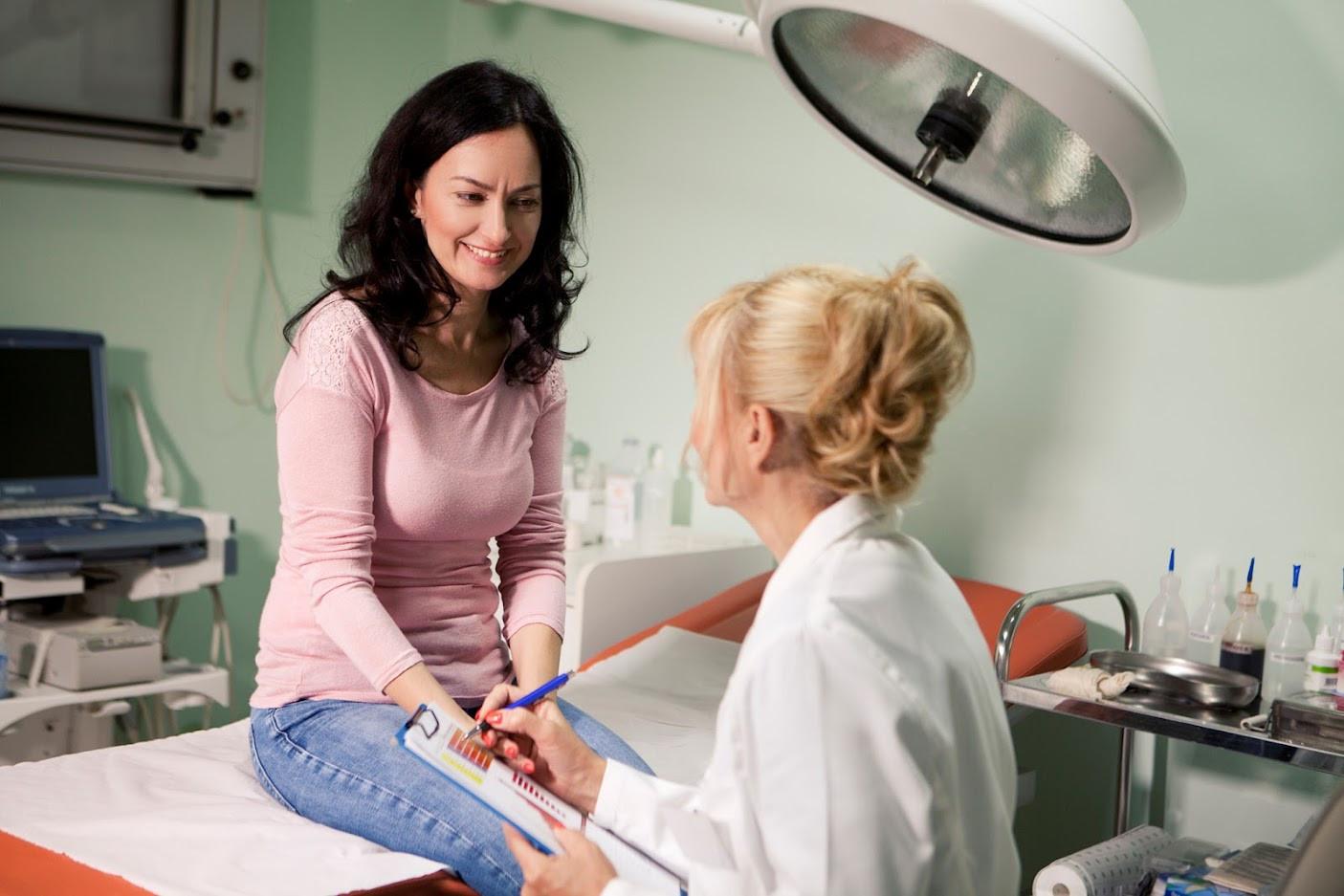
Financial incentives
Find out moreWe encourage general practices to participate in the Practice Incentives Program.
-

Immunisation
Find out moreWe work with primary health care providers to maintain and increase our region’s immunisation coverage rate.
-

Infection control
Find out moreInfection control is vital to providing high quality health care for patients and a safe working environment.
-

MyMedicare
Find out moreMyMedicare is a voluntary patient registration system that aims to formalise the relationship between patients, their general practice, general practitioner and primary care teams.
-

Quality improvement
Find out moreWe can help improve practice workflow with a range of quality improvement tools and resources.
-

Team based care
Find out moreHigh-performing practices view teams as a necessity, ensuring the patient is placed at the centre of their care.
Partnering to integrate services and systems
Integrated care involves providing seamless, effective and efficient care that reflects a person’s health and social care needs. It requires a greater focus on communication and connectivity between healthcare providers, and better access to health services closer to home such as general practice, Aboriginal Community Controlled Health Organisations (ACCHOs) or community-based services.
Collaboration is the key to providing exceptional healthcare, as no single provider can deliver truly integrated care.
-

Working with our Local Health Districts (LHDs)
Find out moreWe have mature and successful partnerships with the LHDs in our region, and we continue to improve service and system integration.
-

Aboriginal Community Controlled Health Organisations (ACCHOs)
Find out moreWe work closely with the four ACCHOs across the region to identify needs, co-design and integrate services.
-

HealthPathways
Find out moreHealthPathways is a a free web-based portal to support general practitioners and health professionals refer patients to the right care, in the right place, at the right time.
-

Specialist Access in the Community Co-design Project
Download File Find out moreThe Specialist Access in the Community Co-design Project aimed to co-design a sustainable, and scalable person-centred model to increase access to specialist care for the residents of South Eastern NSW.
-

The Lumos program
Find out moreThe Lumos program generates new insights to improve health services and patient outcomes across the state.
Learning and development
Work with us to improve local health outcomes
We offer professional development and learning opportunities for health professionals in the region. You can also read about the health needs of South Eastern NSW communities in our Population Health Profile.
To receive the latest health news and upcoming opportunities straight to your inbox, subscribe to our news.
